Introduction
Providing healthcare in remote or rural areas is challenging, particularly specialized medicine and surgical procedures. Patients may need to travel long distances just to get to medical facilities and to communicate with caregivers. They may not arrive in time to receive essential information before their medical appointments and may have to return home before they can receive crucial follow-up care at the hospital. Some patients may wait several days just to meet with their surgeon. This is a very different experience from that of urban or suburban residents or people in more developed areas, where patients can get to a nearby clinic or hospital with relative ease.
In recent years, telemedicine has emerged as a potential solution for underserved remote populations. The COVID-19 pandemic, which prevented many caregivers and patients from meeting in person, helped popularize virtual medical appointments. Yet 2D telemedicine (2DTM) fails to fully replicate the experience of a face-to-face consultation.
To improve the quality of virtual care, researchers from Microsoft worked with external partners in Scotland to conduct the first validated clinical use of a novel, real-time 360-degree 3D telemedicine system (3DTM). This work produced three studies beginning in 2020, in which 3DTM based on Microsoft’s HoloportationTM communication technology outperformed a 2DTM equivalent. Building on the success of this research, the collaborators conducted a follow-up trial in 2022 with partners in Ghana, where they demonstrated the first intercontinental use of 3DTM. This research provides critical progress toward increasing access to specialized healthcare for rural and underserved communities.
3DTM beats 2DTM in Scotland trials
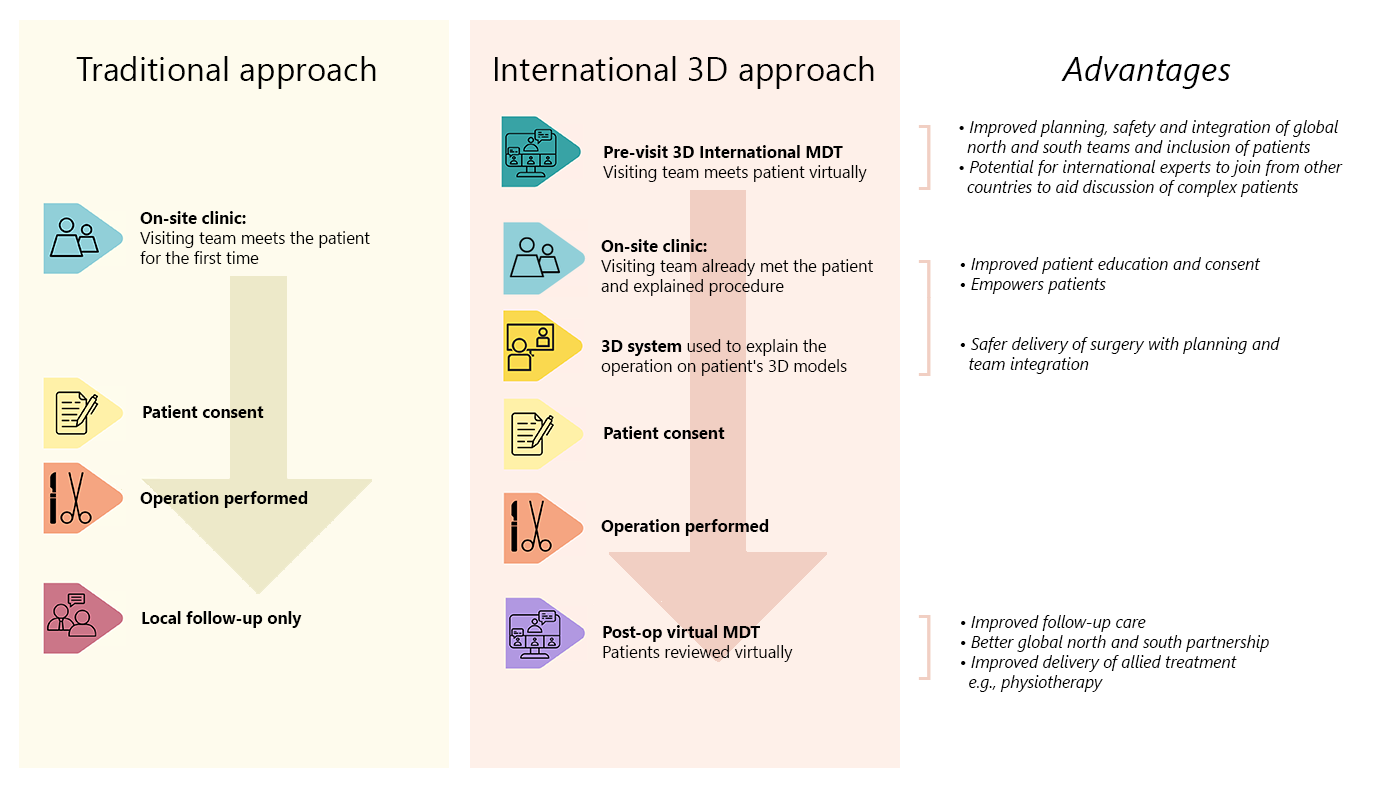
The dramatic expansion of virtual medicine helped fill a void created by COVID restrictions, but it also underscored the need for more realistic remote consultations. While 2DTM can extend the reach of specialized medicine, it fails to provide doctors and surgeons with the same quantity and quality of information they get from an in-person consultation. Previous research efforts had theorized that 3DTM could raise the bar, but the advantages were purely speculative. Until now, real-time 3DTM had been proposed within a research setting only, because of constraints on complexity, bandwidth, and technology.
In December 2019, researchers from Microsoft began discussing the development of a 3DTM system leveraging Microsoft Holoportation communication technology with collaborators from the Canniesburn Plastic Surgery Unit in Glasgow, Scotland, and Korle Bu Teaching Hospital (KBTH) in Accra, Ghana.
communication technology with collaborators from the Canniesburn Plastic Surgery Unit in Glasgow, Scotland, and Korle Bu Teaching Hospital (KBTH) in Accra, Ghana.
With the emergence of COVID-19 in early 2020, this effort accelerated as part of Microsoft Research’s COVID response, with the recognition that it would allow patients, including those with weakened immune systems, to visit a specialist remotely from the relative safety of a local physician’s office, rather than having to travel to the specialist at a hospital with all the concurrent risk of infection.
The initial research included a deployment in Scotland, with 10 specialized cameras capturing patient images, combining them into a 3D model, and transmitting the 3D image to a medical professional. The patient could view the same images as their doctor, which allowed them to discuss them in real time—almost as if they were in the same room.
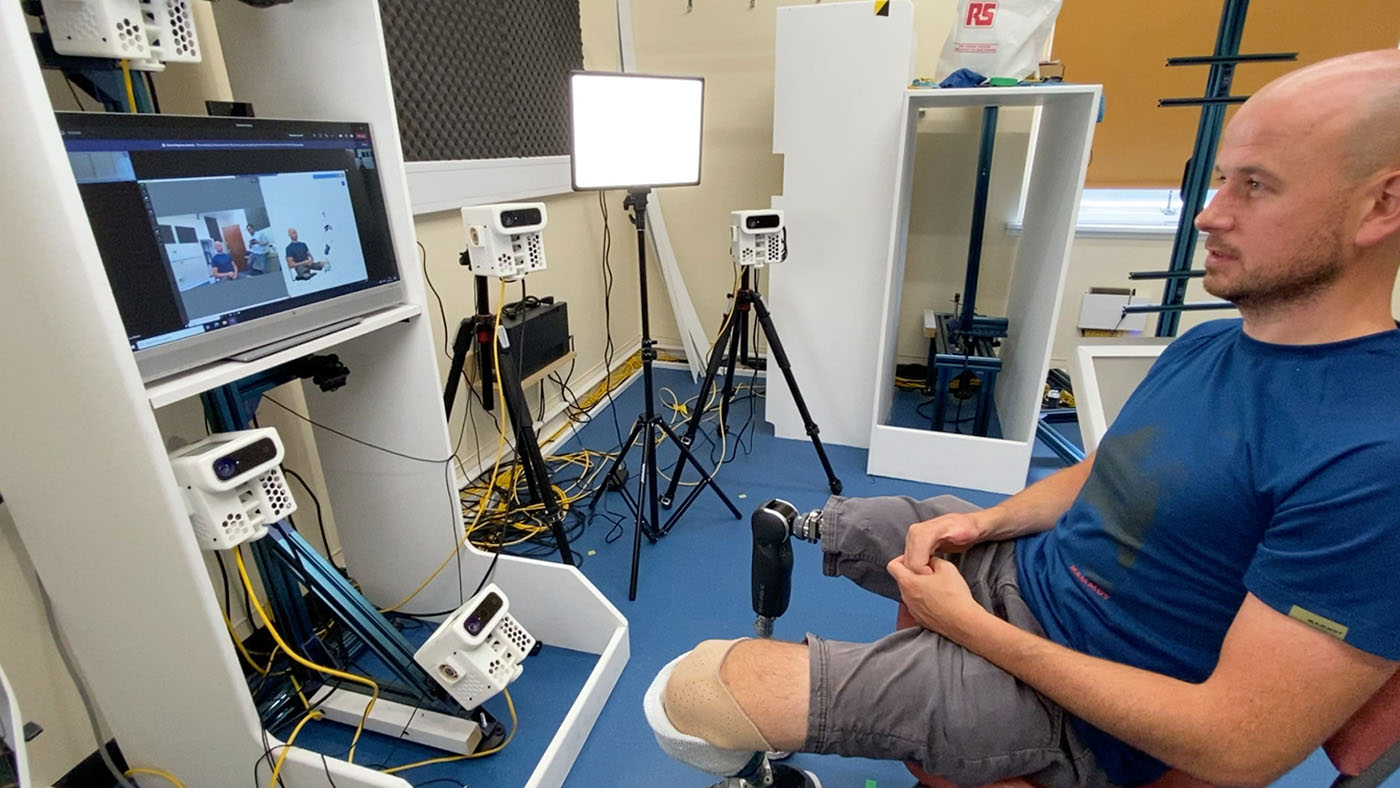
This work produced three separate studies: a clinician feedback study (23 clinicians, November–December 2020), a patient feedback study (26 patients, July–October 2021), and a study focusing on safety and reliability (40 patients, October 2021–March 2022).
Participatory testing demonstrated improved patient metrics with 3DTM versus 2DTM. Although patients still prefer face-to-face visits, 3DTM was rated significantly higher than 2DTM. Overall patient satisfaction increased to 88 percent with 3DTM from 51 percent with 2DTM; realism, or “presence,” rated higher at 80 percent for 3DTM versus 53 percent for 2DTM; and quality as measured by a Telehealth Usability Questionnaire came in at 85 percent for 3DTM compared with 77 percent for 2DTM. Safety and clinical concordance of 3DTM with a face-to-face consultation were 95 percent – equivalent to or exceeding estimates for 2DTM.

One of the ultimate goals of telemedicine is to bring the quality of remote consultations closer to face-to-face experiences. This data provides the first evidence that Microsoft’s Holoportation communication technology moves 3DTM closer to this goal than a 2D equivalent.
communication technology moves 3DTM closer to this goal than a 2D equivalent.
“We showed that we can do it using off-the-shelf components, making it affordable. And we can deploy it and make it reliable enough so that a doctor or a clinical team could use it to conduct consultations,” said Spencer Fowers, Principal Researcher at Microsoft Research.
Ghana study: 3DTM brings doctors and patients closer
After the successful deployment in Scotland, the team turned its focus to Ghana. The research team visited KBTH in February 2022. That began the collaboration on the next phase of the project and the installation of the first known 3D telemedicine system on the African continent.
Ghana has a population of 31 million people but only 16 reconstructive surgeons, 14 of whom work at KBTH. It’s one of the largest hospitals in west Africa and the country’s main hospital for reconstructive surgery and burn treatment. Traveling to Accra can be difficult for people who live in rural areas of Ghana. It may require a 24-hour bus ride just to get to the clinic. Some patients can’t stay long enough to receive follow-up care or adequate pre-op preparation and counseling. Many people in need of surgery never receive treatment, and those that do may receive incomplete or sub-optimal follow-up care. They show up, have surgery, and go home.
“As a doctor, you typically take it for granted that a patient will come back to see you if they have complications. These are actually very complex operations. But too often in Ghana, the doctors may never see the patient again,” said Stephen Lo, a reconstructive surgeon at the Canniesburn Plastic Surgery and Burns Unit in Scotland. Lo has worked for years with KBTH and was the project’s clinical lead in Glasgow.
The researchers worked with surgical team members in Scotland and Ghana to build a portable system with enhanced lighting and camera upgrades compared to the original setup deployed in Scotland. This system would enable patients to meet in 3D with doctors in Scotland and in Ghana, both before and after their surgeries, using Microsoft Holoportation communication technology.
communication technology.
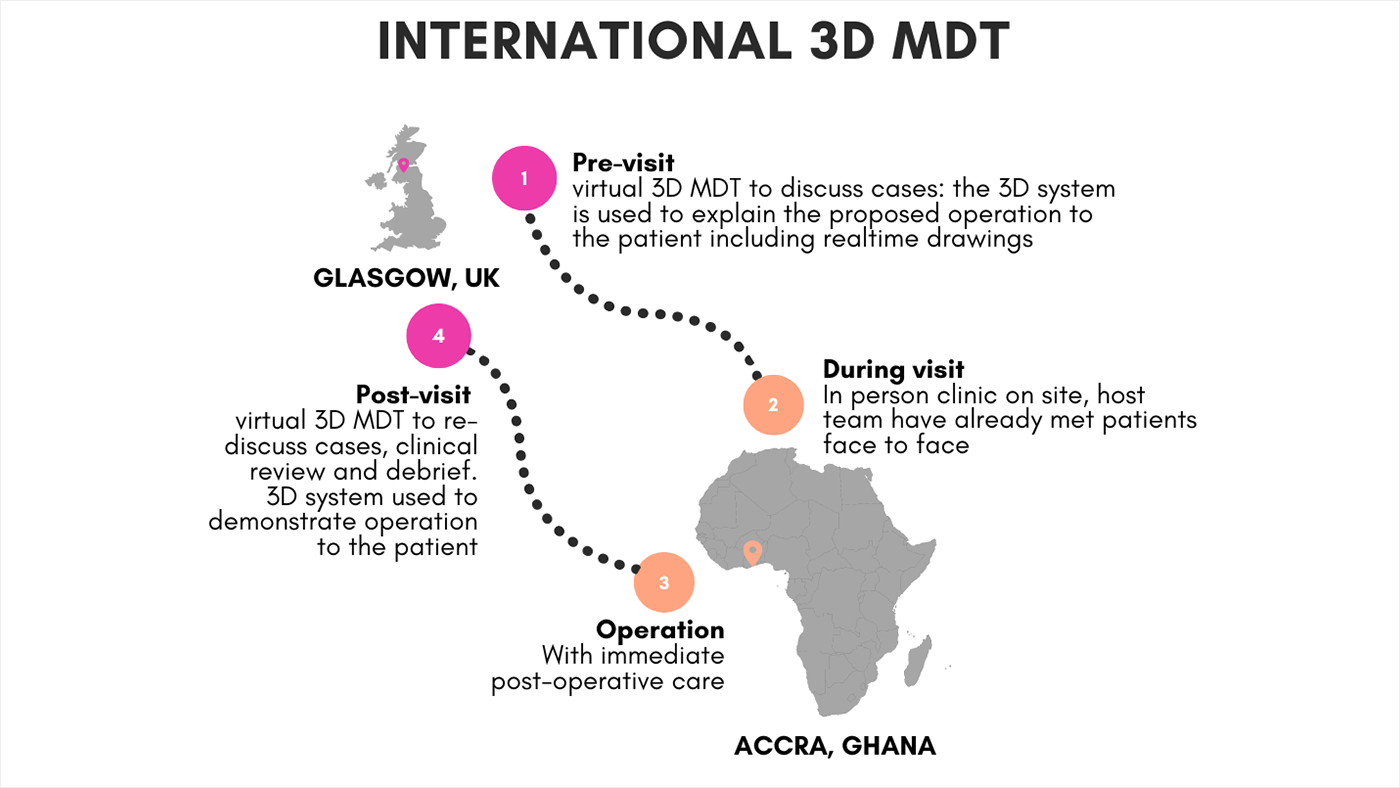
The results were multiple successful multidisciplinary team (MDT) engagements—both pre-operative and post-operative—supporting surgeries led by visiting doctors from Scotland at KBTH. The 3DTM system using Microsoft Holoportation communication technology helped doctors communicate to patients precisely what their surgery would entail ahead of time and then ensure that patients had access to any necessary follow-up procedures and post-operation therapy. The medical team in Glasgow used Microsoft Holoportation
communication technology helped doctors communicate to patients precisely what their surgery would entail ahead of time and then ensure that patients had access to any necessary follow-up procedures and post-operation therapy. The medical team in Glasgow used Microsoft Holoportation communication technology to manipulate and mark up 3D images of their patients. Patients watching from Accra could visualize the procedure, including the exact locations where the surgical incisions would occur.
communication technology to manipulate and mark up 3D images of their patients. Patients watching from Accra could visualize the procedure, including the exact locations where the surgical incisions would occur.
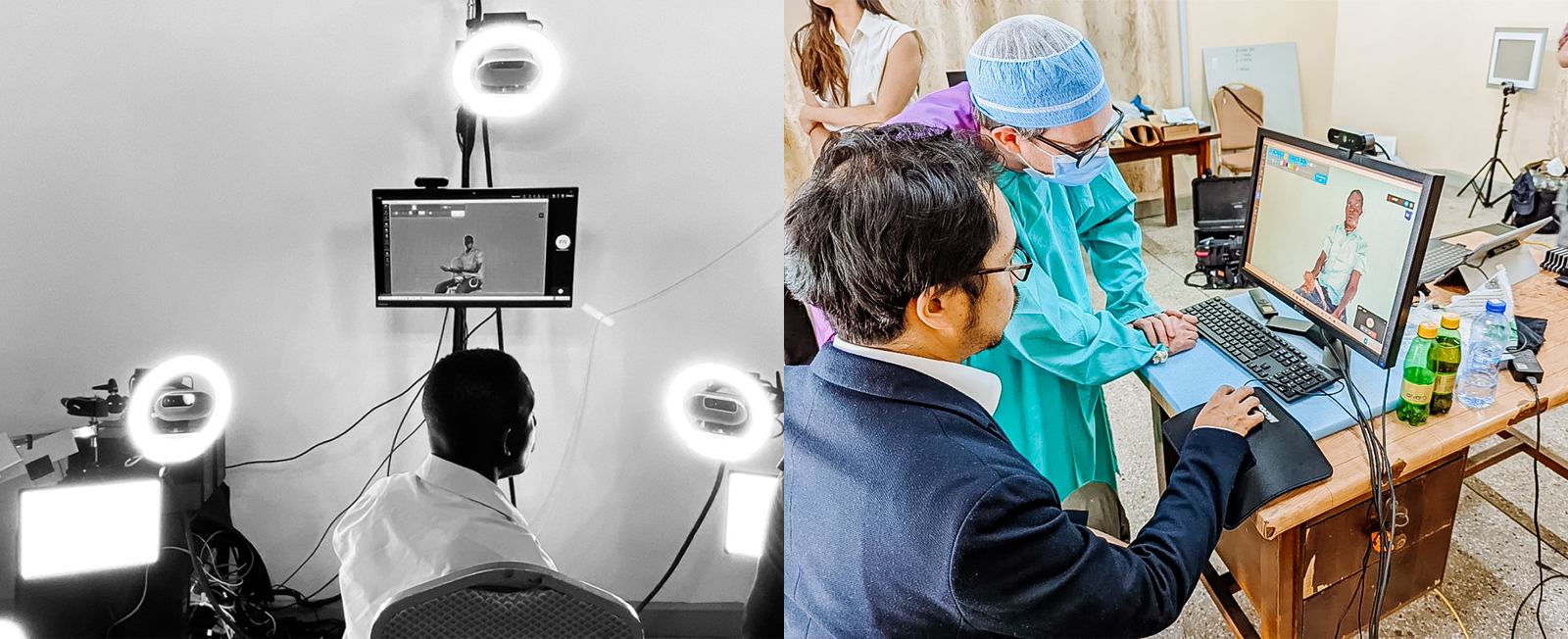
For a patient who came to KBTH to address a chronic problem with his jaw, this visualization gave him a much better understanding than he had had with previous surgeries, said Levi Ankrah, a reconstructive surgeon at KBTH who participated in the remote consultations and the surgeries in Ghana.
“These are quite complex things to explain. But when the patient could actually see it for himself from the outside, that helped him feel more involved with his care and his follow-up plan,” Ankrah said.
Conclusion
One of the ultimate goals of telemedicine is for the quality of remote consultations to get closer to the experience of face-to-face consultations. The data presented in this research suggests significant potential in moving closer to the experience of face-to-face consultations, which is particularly relevant to specialties with a strong 3D focus, such as reconstructive surgery.
Nothing can replace the authenticity and confidence that come from a face-to-face visit with a doctor. But 3DTM shows great promise as a potential state-of-the-art solution for remote telemedicine, replacing current 2DTM virtual visits and driving better access and outcomes for patients.
Acknowledgments
We would like to acknowledge the following contributors to this project: Andrea Britto; Thiago Spina; Ben Cutler; Chris O’Dowd; Amber Hoak; Spencer Fowers; David Tittsworth; Whitney Hudson; Steven Lo, Canniesburn Regional Plastic Surgery and Burns Unit, Glasgow; Kwame Darko, Levi Ankrah, and Opoku Ampomah, National Reconstructive Plastic Surgery and Burns Center, Korle Bu Teaching Hospital, Accra.
Additional thanks to: Korle Bu Teaching Hospital, NHS Scotland West of Scotland Innovation Hub, Canniesburn Plastic Surgery and Burns Unit.

On the right, in medical gear (from left to right): Chris O’Dowd, Kwame Darko, Thiago Spina, Andrea Britto and Spencer Fowers.
The post 3D telemedicine brings better care to underserved and rural communities, even across continents appeared first on Microsoft Research.
